 Cardiopulmonary exercise testing and radionuclide ventriculogram were also performed where possible. Relevant data from 241 CHF patients were analysed retrospectively. The purpose of this study was (a) to identify the best ECG parameter that predicts mortality, (b) to evaluate the prognostic marker of ECG against well-established indicators of prognosis. This method obtained a high rate of S-V interval and LBBP owing to the simultaneous use of John Jiang’s connecting cable.Chronic heart failure (CHF) is associated with high mortality, and there are several established clinical and laboratory parameters that predict mortality in CHF. Low-output shortening of the S-peak LVAT predicted the S-V interval with 100% sensitivity and 33.3% specificity. However, in the majority of patients (25/28, 89.29%), the S-V interval was observed after the shortening of the S-peak LVAT at continuous low output. In this study, none of the patients presented the S-V interval by reducing the output after the shortening of the S-peak LVAT at low and high output. More importantly, the parameters of the 2 shortenings (the S-peak LVAT before shortening, the S-peak LVAT after shortening, and the duration of shortening) all showed significant positive correlation (PCC = 0.915, P <. Continuous low-output pacing is performed to confirm whether the consecutive low output can shorten the S-peak LVAT, which indicates the capture of the left conduction system. High output shortens the S-peak LVAT, which indicates that the tip electrode of the LBBP lead is adjacent to the left conduction system. This method was found to reduce the risk of acute ventricular septal perforation (incidence: 1/28, 3.57%) and lead dislocation (incidence 0%) during the procedure. At the completion of the procedure, the mean unipolar LBBP threshold and sensing of the R wave were 0.42 ± 0.14 V and 13.61 ± 4.67 mV, respectively. Patients who exhibited abrupt change was observed 2 times in S-LVAT had higher myocardium threshold (mean: 1.19 ± 0.46 V) than the LBB threshold (mean: 0.68 ± 0.37 V). However, none of the patients showed S-V interval after abrupt change at high and low outputs (5 V / 0.5 ms and 2 V / 0.5 ms pacing). Abrupt change was observed 2 times in S-peak LVAT (at 5 V / 0.5 ms and 2 V / 0.5 ms pacing 2 V / 0.5 ms continuous pacing) was observed in 96.43% of patients S-V interval appeared after the abrupt change at low output (2 V / 0.5 ms continuous pacing) in 89.29% by rapidly reducing the output. All patients presented RBBB morphology during pacing. LBBAP was unsuccessful in 1 patient with a large atrium. Twenty-seven of the 28 (96.43%) patients received LBBAP successfully. The procedural parameters and characteristics of the study population are shown in Table 2. 
The depth of the lead position inside the LV septum was estimated by radiography with contrast injection in the left anterior oblique 45° projection. At the same time, the output was rapidly reduced, and the intracardiac paced QRS morphology was recorded by the LBBP lead. When the first abrupt shortening by adjacent paced beats with the low output (2 V / 0.5 ms) was longer than 10 ms, the operator stopped screwing the tip of the LBBP lead ( Figure 3). 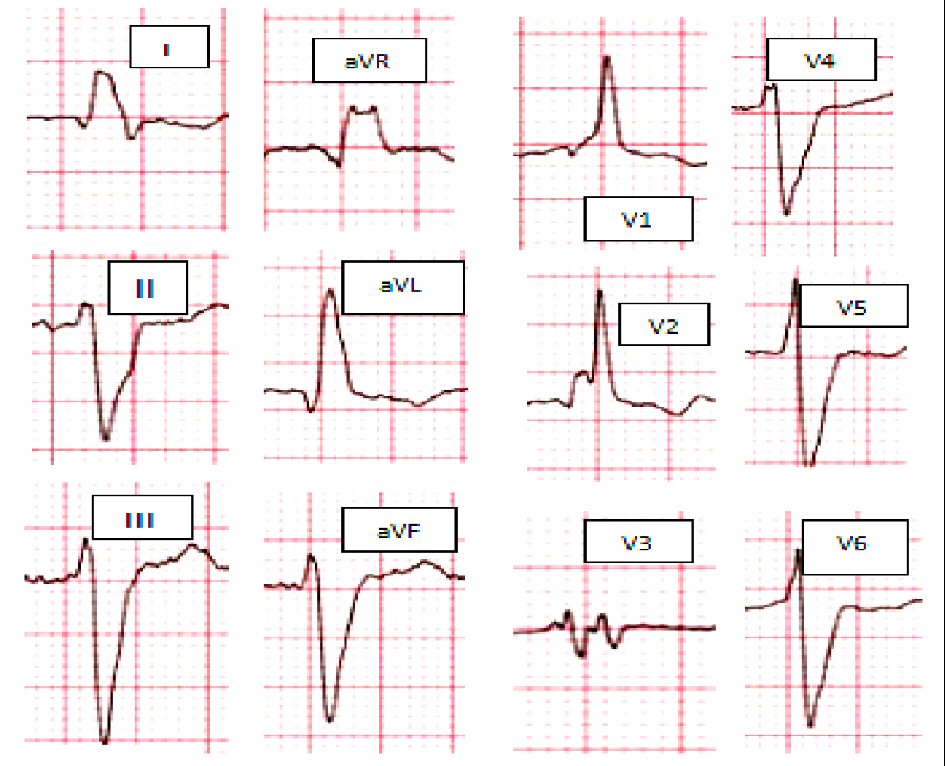
Continuous unipolar pacing at low output (2 V / 0.5 ms) was performed during the subsequent period of LBBP lead implantation. The duration of the pacing S-peak LVAT in lead V 5 was measured with LBBP lead pacing. With the abrupt shortening between the stimulation signal and peak LV activation (S-peak LVAT) in lead V5, LBBP lead continued to be screwed slightly ( Figure 2). The impedance of the tip electrode of the LBBP lead was monitored discontinuously at high output (5 V / 0.5 ms). With advancement of the helix into the interventricular septum, the mid notch shifted toward the end of the QRS wave in lead V 1. 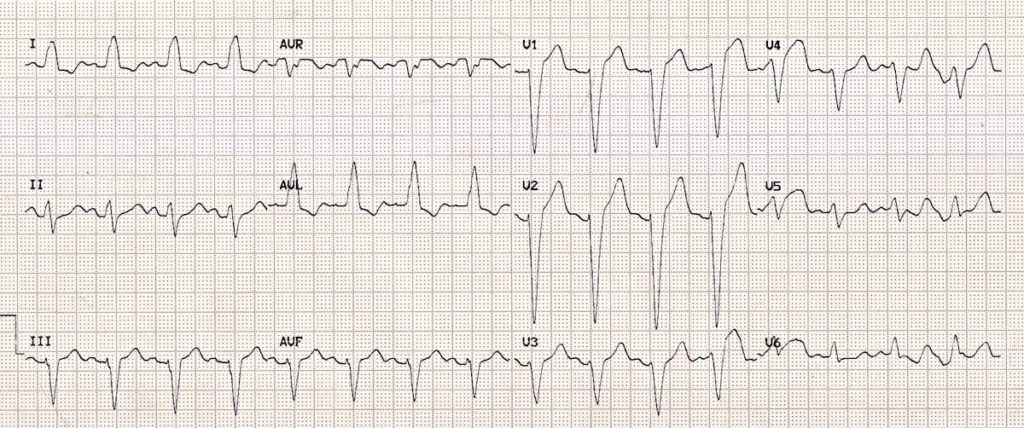
When the tip of the pacing lead was fixed at the septum, the paced QRS morphology usually demonstrated a “W” shape with a mid notch in lead V 1. John Jiang’s connecting cable was connected with the lead for pace mapping at low output (2 V / 0.5 ms). In the right anterior oblique 30° view, the lead with sheath was advanced from the right side of the septum to the left side. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
